Bristol Woman Convicted of Defrauding Medicaid Program
Deirdre M. Daly, United States Attorney for the District of Connecticut, Phillip Coyne, Special Agent in Charge for the U.S. Department of Health and Human Services, Office of Inspector General, and Chief State’s Attorney Kevin T. Kane today announced that on May 26, a jury in Bridgeport convicted RONNETTE BROWN, 44, of Bristol, on 23 counts of health care fraud and one count of conspiracy to commit health care fraud. The trial before U.S. District Judge Victor A. Bolden began on May 22 and the jury returned a verdict of guilty on all counts of the indictment on Friday afternoon.
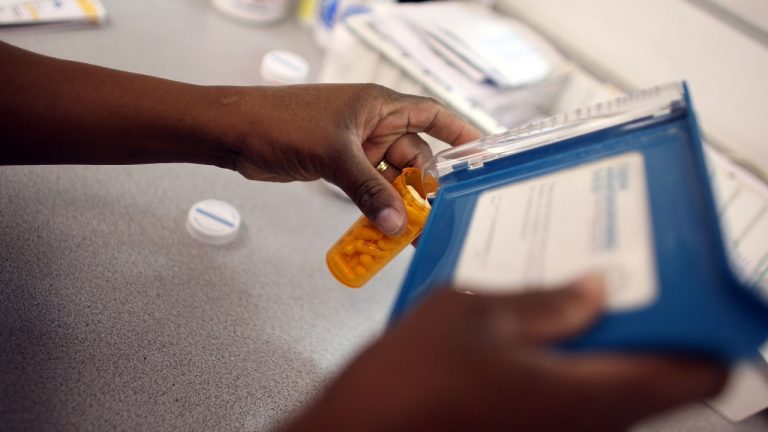
According to the evidence at trial, Brown owned and operated WeMPACT, LLC, a social services business with offices in Bristol and Torrington. Between August 2010 and April 2014, Brown billed Medicaid for psychotherapy services that were not performed. In addition to that scheme, Brown separately conspired with Beverly Coker and another unnamed individual to bill Medicaid for psychotherapy services that represented Coker had performed the services when, in fact. the services were provided by unlicensed individuals, or were not provided at all.
According to court documents and statements made in earlier court proceedings, Coker, a licensed clinical social worker, owned and operated New Beginnings Family Center, LLC, in Hartford. On April 8, 2016, Coker, of Windsor, waived her right to indictment and pleaded guilty to one count of health care fraud, admitting that between October 2010 and November 2011, she engaged in a scheme to defraud Medicaid by permitting Brown and another individual to bill Medicaid for psychotherapy services using Coker’s Medicaid provider number. The services were either performed by unlicensed individuals or not performed at all. Under the scheme, Coker kept 30 percent of the proceeds, and paid the remaining 70 percent to Brown and the other individual. As part of her plea, Coker admitted to defrauding Medicaid of approximately $214,555 through the scheme.
Judge Bolden scheduled sentencing for August 18, 2017, at which time Brown faces a maximum term of imprisonment of 10 years on each count of health care fraud, and a maximum term of imprisonment of five years on the conspiracy count. She has been released on a $100,000 bond since her arrest on May 23, 2016.
Coker awaits sentencing. Three other individuals were charged and convicted of health care fraud offenses stemming from this investigation.
“This conviction is the latest example of the successful efforts of the Connecticut Medicaid Fraud Working Group,” said Attorney Daly. “Through that group, federal and state law enforcement and representatives of state agencies combine our efforts to detect, investigate, and prosecute Medicaid fraud through criminal and civil prosecutions. In this particular case, federal agents worked alongside our partners from the Medicaid Fraud Control Unit of the Chief State’s Attorney’s Office, and were supported by the State Attorney General’s Office and the Connecticut Departments of Health (DPH) and Social Services (DSS). This seamless coordination ensures that the Connecticut Medicaid program is protected from unscrupulous providers. We look forward to continuing the teamwork with our state and federal partners to ensure that every dollar spent by the Medicaid program goes to provide much-needed medical services to Medicaid clients.”
“Being a health care provider in the Medicaid program is a privilege, not a right,” said HHS-OIG Special Agent in Charge Coyne. “When Ronnette Brown conspired to enrich herself by billing the government for services never provided or provided by unqualified professionals, she violated the basic trust that taxpayers extend to healthcare professionals. Our agents continue to work with Medicaid Fraud Control Units to root out such fraud schemes, which undermine the financial health of government health care programs and the public’s trust in medical professionals.”
“This is yet another example of how much we can achieve when agencies at all levels of government work together in collaboration,” said Chief State’s Attorney Kane. “This conviction will hopefully put all health care providers on notice that we are committed at all levels of government to detecting, investigating and prosecuting fraud that steals scarce resources from the programs that serve people in need.”
This matter has been jointly investigated by the Office of the Inspector General of the U.S. Department of Health and Human Services and the Medicaid Fraud Control Unit of the Chief State’s Attorney’s Office, with assistance from the Connecticut Attorney General’s Office. U.S. Attorney Daly also thanked the Connecticut Department of Social Services for their role in identifying the fraudulent scheme and supporting the investigation and prosecution of the case.
The U.S. Attorney’s Office, Chief State’s Attorney’s Office and Attorney General’s Office meet regularly as part of The Medicaid Fraud Working Group. The Working Group also includes representatives from the Connecticut Department of Social Services; the Connecticut Department of Public Health; the Drug Control Division of the Connecticut Department of Consumer Protection; the Office of the Inspector General of the U.S. Department of Health and Human Services, and the FBI. The Working Group reviews pending issues and cases, identifies trends that might indicate fraudulent activity, and coordinates efforts for maximum results.
This matter is being prosecuted by Assistant U.S. Attorneys David J. Sheldon and Christopher W. Schmeisser.
People who suspect health care fraud are encouraged to report it by calling 1-800-HHS-TIPS.